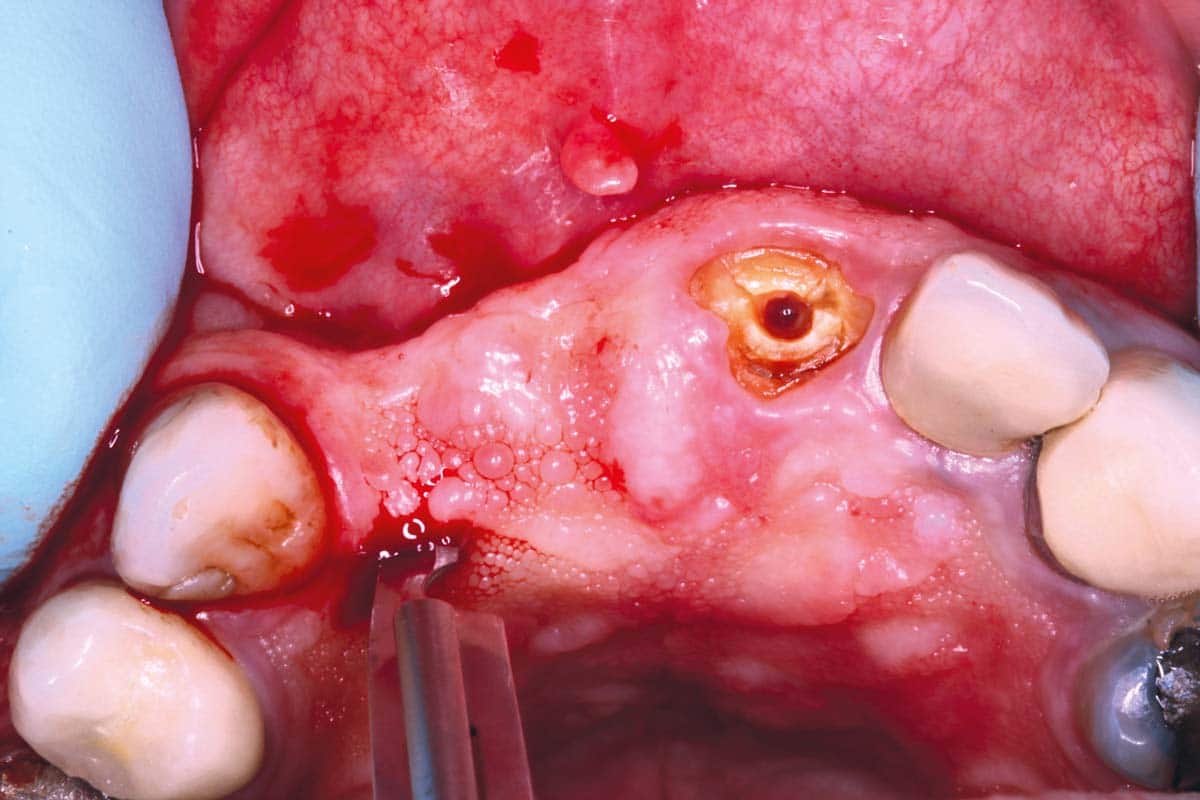
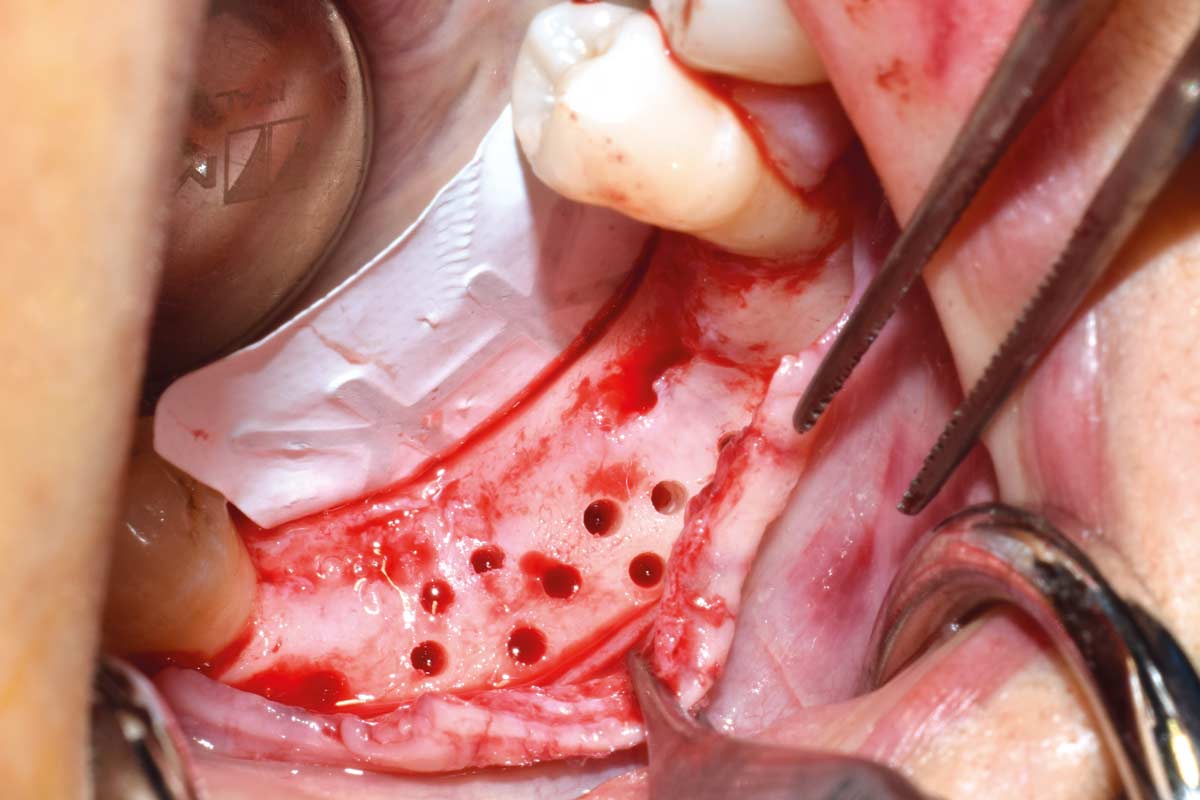
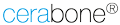MEMBRANE TECHNIQUES
cerabone® can be used in conjunction with all types of barrier membranes (non-resorbable and resorbable membranes) and all common surgical- as well as membrane techniques.
Resorbable devices like collagen membranes omit the need for a second surgery for removal. Porcine collagen membranes like Jason® membrane and collprotect® membrane have demonstrated excellent biocompatibility and provide an efficient barrier function for many treatment concepts in GBR and GTR procedures with cerabone®1,2.
Non-resorbable membranes offer a greater form stability than resorbable devices and are therefore the first the first choice for the treatment of bone defects outside the bony envelope. PTFE membranes like permamem® provide the required space and time for the complete regeneration of the augmented sites3.
IN CONJUNCTION WITH
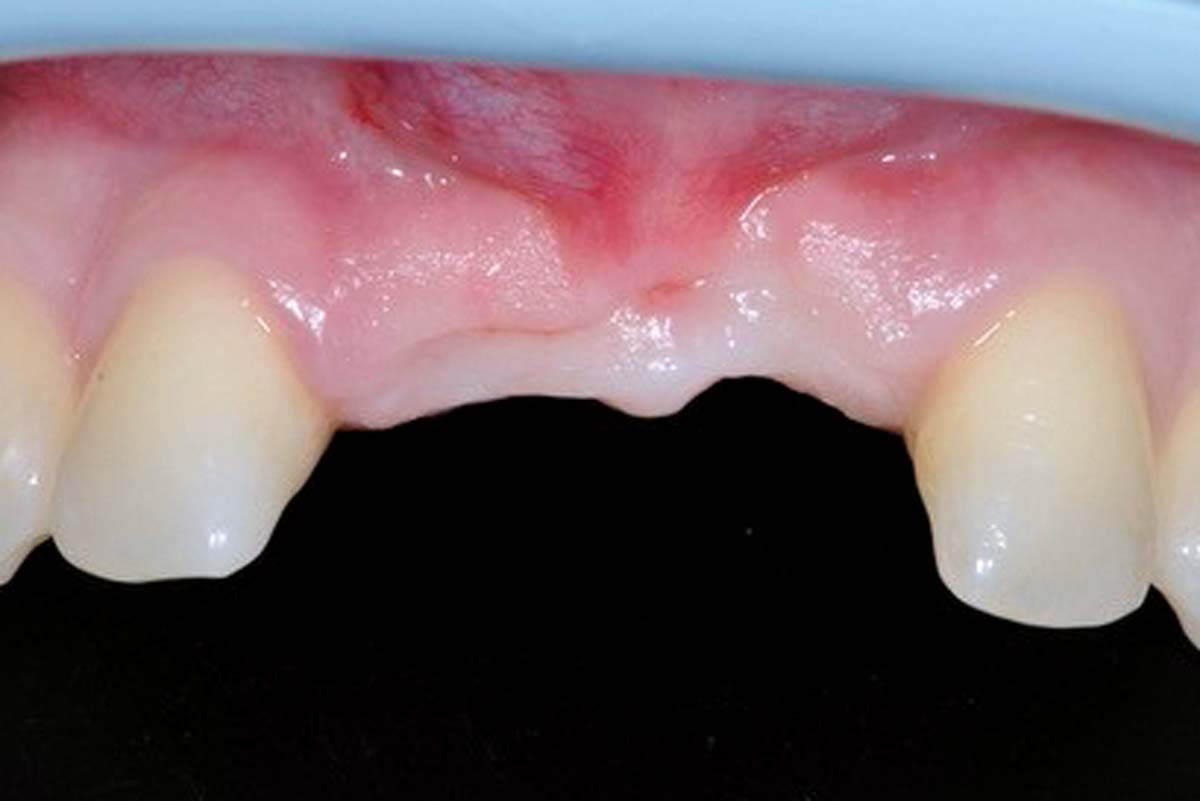
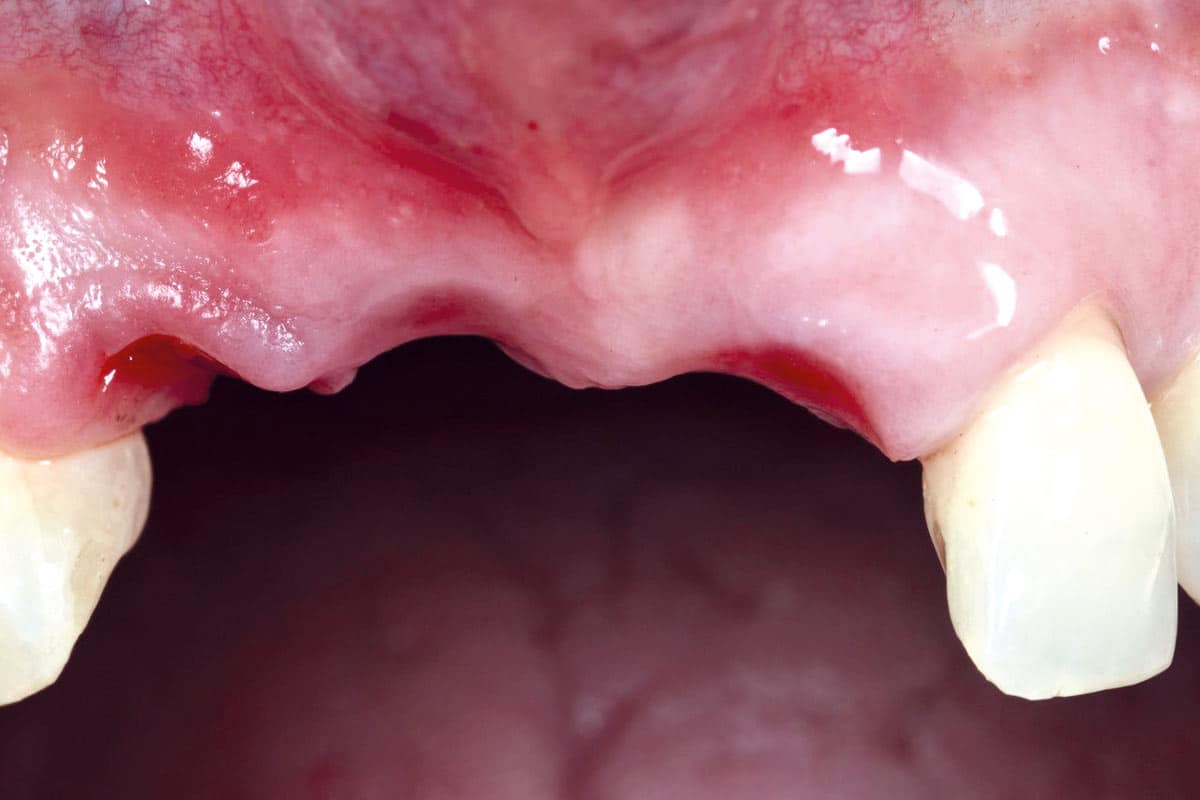
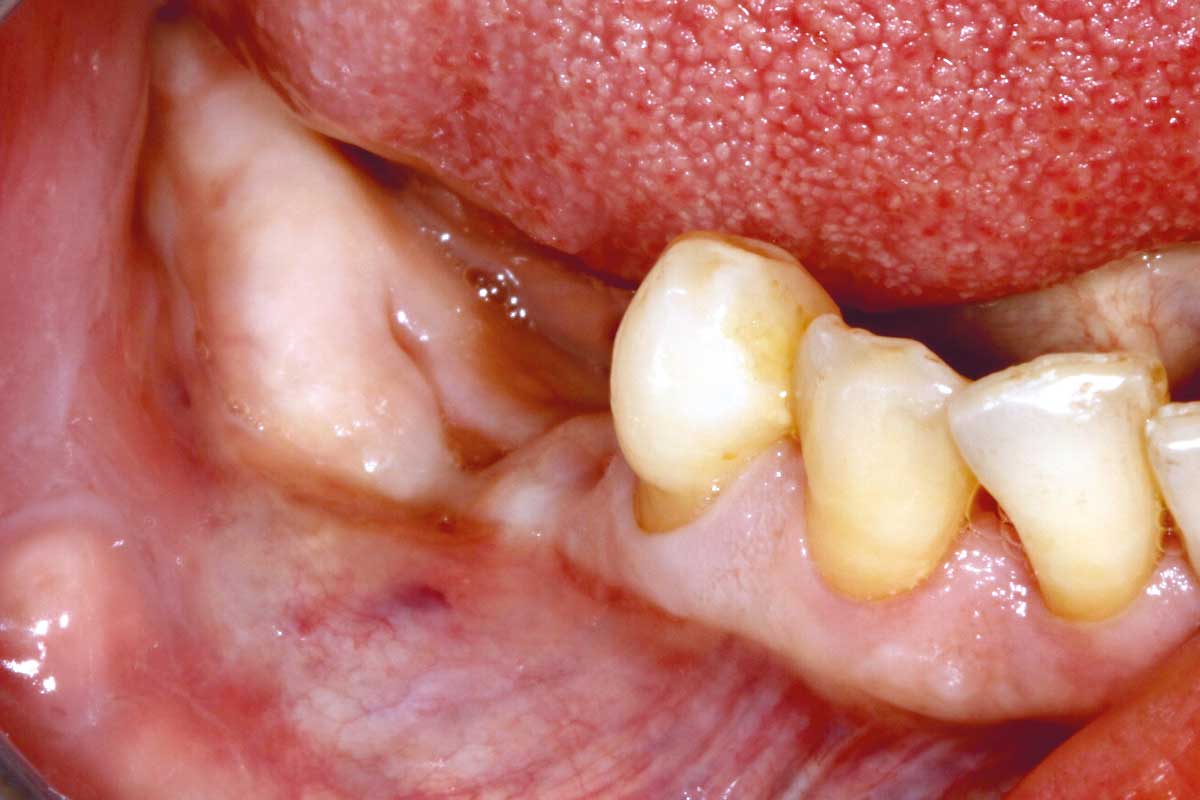
COMBINATION cerabone® & Jason® membrane
cerabone® and Jason® membrane combine all the properties required for successful Guided Bone Regeneration.
cerabone® provides a long-term stable scaffold for new bone formation, while Jason® membrane ensures an undisturbed and complete bone maturation by providing a sufficient barrier time4-8.
The excellent biomechanical properties together with the specific resorption profile of Jason® membrane optimally support both, early healing of the cerabone®-grafted area, and the long-term stable integration of the particles.
Histological analyses have revealed that Jason® membrane efficiently prevents soft tissue ingrowth into the cerabone®-augmented site, thus enabling optimal integration of the particles into newly formed bone matrix9.
The multidirectional strength and tear resistance of Jason® membrane permit well securing of the cerabone® particles at the augmented site providing optimal regenerative conditions even in challenging situations8.
Jason® membrane
NATIVE PERICARDIUM MEMBRANE
Jason® membrane is a particularly thin, native collagen membrane obtained from porcine pericardium that provides a long barrier function.
Owing to the unique biomechanical properties of the pericardium, the membrane exhibits a remarkable tear resistance as well as excellent surface adaptation.
PROPERTIES
– Naturally long barrier function
– Multi-directional strength and tear resistance
– No stickiness after hydration
– Excellent surface adaptation
– Easy manipulation
– Can be applied dry or wet
– Low thickness, no swelling upon hydration
INDICATIONS:
Implantology, Periodontology and Oral and CMF Surgery
– Horizontal and vertical augmentation
– Ridge reconstruction
– Socket and ridge preservation
– Sinus lift
– Protection and covering of Schneiderian membrane
– Fenestration and dehiscence defects
– Intraosseous defects (1 to 3 walls)
– Furcation defects (class I and II)
PRODUCT LINE
| Art.-No. | Size | Content |
|---|---|---|
| 681520 | 15 × 20 mm | 1 membrane |
| 682030 | 20 × 30 mm | 1 membrane |
| 683040 | 30 × 40 mm | 1 membrane |
pinned or sutured
high tear resistence
very thin

Millions of patients treated

> 20 years clinical experience
in various medical applications

in > 90 countries

> 200 scientific contributions
REFERENCES
1 Ohayon L, Taschieri S, Friedmann A, Del Fabbro M. Bone Graft Displacement After Maxillary Sinus Floor Augmentation With or Without Covering Barrier Membrane: A Retrospective Computed Tomographic Image Evaluation Int J Oral Maxillofac Implants. 2019 May/June;34(3):681–691.
2 Rothamel D, Schwarz F, Fienitz T, Smeets R, Dreiseidler T, Ritter L, Happe A, Zöller J. Biocompatibility and biodegradation of a native porcine pericardium membrane: results of in vitro and in vivo examinations. Int J Oral Maxillofac Implants. 2012 Jan-Feb;27(1):146-54.
3 González-Ruiz, A., Gómez Menchero, A., Ríos, J.V, Bullón, P., Lázaro Calvo, P. Lateral bone augmentation with xenograft blocks: what could we achieve? Poster EuroPerio Amsterdam 2018.
4Tawil G, Tawil P, Khairallah A. Sinus Floor Elevation Using the Lateral Approach and Bone Window RepositioningI: Clinical and Radiographic Results in 102 Consecutively Treated Patients Followed from 1 to 5 Years. Int J Oral Maxillofac Implants. 2016 Jul-Aug;31(4):827-34.
5 Forna, D.A. & Forna, Norina & Earar, K & Popescu, E. (2017). Postoperative clinical evolution of edentulous patients treated by guided bone regeneration using xenograft bone substitute and collagen membrane. Materiale Plastice. 54. 312-315.
6 Arab S, Reza Arab H, Aghaloo M, Shiezadeh F, Tajik S, Moeintaghavi A. (2018). Periosteal Envelope Flap as a Technique for Horizontal Bone Augmentation: A Case Series Study. The Open Dentistry Journal. 12. 995-1003.
7 Samieirad S, Eshghpour M, Tohidi E, Jouya A, Soufizadeh R, Kermani H. Using Absorbable Gelatin Sponge to Facilitate Sinus Membrane Elevation during Open Sinus Lift: Technical Notes and Case Series. Journal of Dental Materials and Techniques, 2018; (): 1-7.
8 Khojasteh A, Hosseinpour S, Rad MR, Alikhasi M. Buccal Fat Pad-Derived Stem Cells in Three-Dimensional Rehabilitation of Large Alveolar Defects: A Report of Two Cases. J Oral Implantol. 2019 Feb;45(1):45-54.
9 Rothamel D, Schwarz F, Fienitz T, Smeets R, Dreiseidler T, Ritter L, Happe A, Zöller J. Biocompatibility and biodegradation of a native porcine pericardium membrane: results of in vitro and in vivo examinations. Int J Oral Maxillofac Implants. 2012 Jan-Feb;27(1):146-54.